For any questions:
A definition of immunotherapy
Immunotherapy was first used as a cancer treatment about a century ago. A few early studies revealed that deliberately infecting certain cancer patients stimulated their immune system and positively impacted their cancer. As science progressed and effective and accessible treatments such as chemotherapy and radiotherapy were developed, immunotherapy was temporarily shelved. The first trials aimed at prompting the immune system to act on cancer tumors were performed in the 1950s, after which came immune system interventions such as bone marrow transplants.
Immune system stimulation as a means of destroying cancer tumors was thrust into the spotlight in the early 2000s, and quickly proved a promising avenue for scientific research.
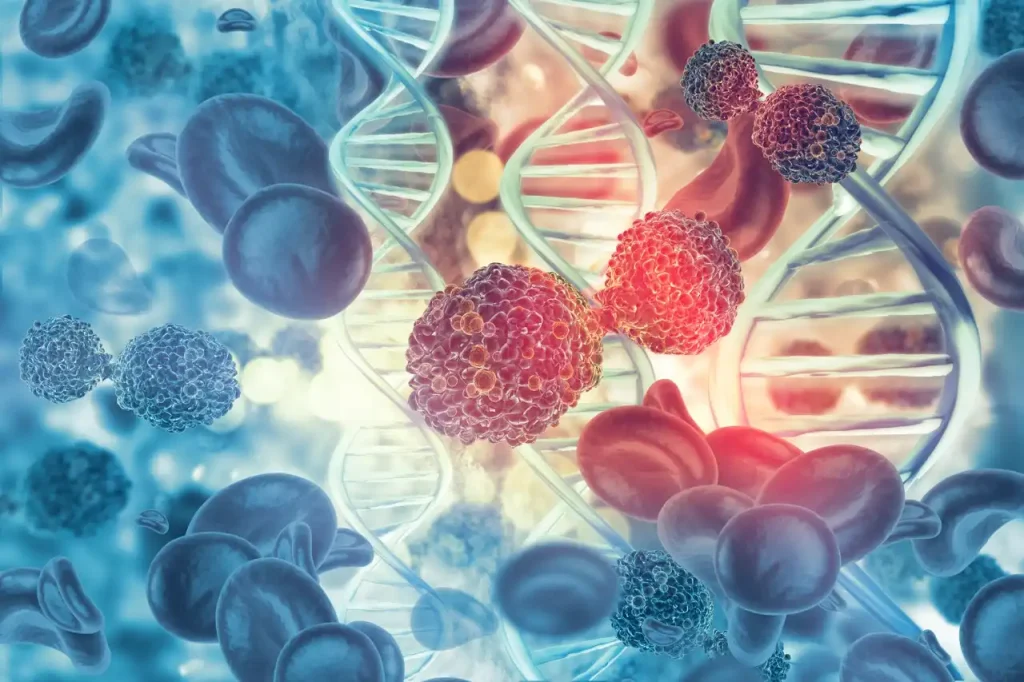
Immunotherapy is now on the verge of becoming one of the cornerstones of modern-day oncology, with various parties speaking of advanced immunotherapy and personalized or precision medicine. But to better grasp the role of immunotherapy in an oncology setting, we need to first understand the workings of the human immune system.
What is the immune system?
The role of the immune system is to protect the body.
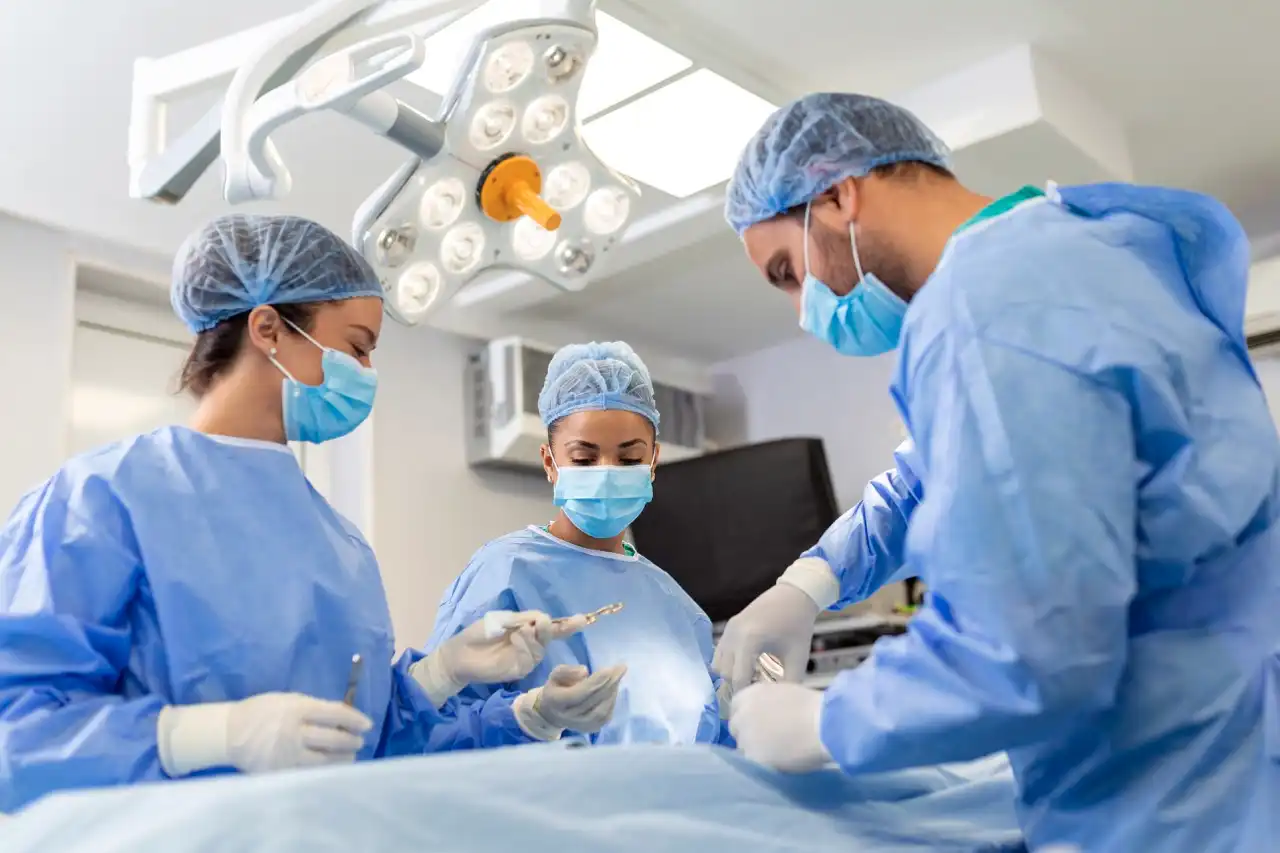
What is immunotherapy in oncology?
It is a treatment that allows the body’s cells to fight cancer cells more effectively.
Types of drugs or immunotherapy treatments in oncology
Interferon alpha (Intron A, Wellferon), interleukin-2 (Proleukin), intravesical bacillus Calmette-Guérin (BCG) treatment, immune checkpoint inhibitors…
Receiving immunotherapy, which treatment for which cancer?
Immunotherapy is a very active area of research. There are several types of treatments for the same cancer and for different cancers.
Primary cancers treated with immunotherapy
With the recent development of many immunotherapies, including checkpoint inhibitors, several types of cancers are treated with immunotherapy.
Side effects of the primary immunotherapy treatments
Immunotherapy treatments in oncology can have side effects that are significantly different from those of other cancer treatments such as chemotherapy or radiotherapy.
Sources
Institut National du Cancer – Médecine de précision : thérapies ciblées et immunothérapie spécifique
Canadian Cancer Society – Immunotherapy
American Cancer Society – Immunotherapy
La ligue contre le cancer – L’immunothérapie
National Cancer Institute – Immunotherapy to Treat Cancer
Guides prepared for patients :
European Society for Medical Oncology – Les effets secondaires liés à l’immunothérapie
Société leucémie et lymphome Canada – L’immunothérapie
CHUM – L’immunothérapie pour traiter le cancer
All of the sources used to prepare this document can be consulted by communicating with the Quebec Cancer Foundation.
To find out more
To obtain more detailed information on immunotherapy and some tips on how to feel better, call the Info-cancer Hotline at 1-800-363-0063 to talk to a nurse or documentalist.
Borrow one or more books on the subject free of charge from our Info-cancer Library (available in French only).